More than 12 million people in the United States have Restless Legs Syndrome.
Creepy-crawly, tingly, itchy, achy legs are a regular nightly occurrence for people who have Restless Legs Syndrome (RLS). The National Institute of Neurological Disorders and Stroke estimates that 7-10% of the entire population of the United States have restless leg syndrome, and it is also highly likely that many people who have the condition go undiagnosed. Even more significant is the impact it has on your life. People describe the symptoms as disturbing and unbearable, and people always have poor-quality sleep which affects their overall health. That’s why the pursuit of a diagnosis and an effective treatment plan is such an important priority for sufferers.
A Connection Between Restless Legs Syndrome and a Vein Condition
In my experience as a vein specialist over the past 16 years, I have treated patients on a daily basis who suffer from RLS and its effects. Over the years, I and other vein specialists have noted a correlation between restless leg syndrome and vein reflux - and the symptoms and patterns match. In the majority of my patients who suffer from RLS, and who also are found to have a vein condition, their symptoms significantly improve or disappear with treatment.
It’s more than a passing coincidence. On this page, I will discuss the correlation that I see between vein reflux and RLS and how vein treatments can help. I’ll also discuss the treatments and talk about the benefit derived from alleviating the symptoms. My goal is to share what I’ve learned in over 15 years of treating vein conditions and over 10 years as a cardiac and vascular surgeon. I also suffered from a vein condition and restless legs and know firsthand how debilitating symptoms can be and how exhilarating it is when symptoms go away after treatment. For these reasons, I am excited to share what I have learned and offer hope to those who suffer from RLS.
One patient named Jim, in particular, said that, after treatment for his vein condition, his RLS symptoms went away and he was able to sleep through the night for the first time in 25 years. Before that, he got at most 4 hours of sleep, and he felt tortured by it.
Most patients I see are frustrated by their restless leg symptoms and lack of relief with conventional medical therapy. Most primary care providers, including neurologists, have not yet been exposed to the growing awareness amongst vein care practitioners that there is a vein source for many patients with Restless Legs Syndrome, and treatments do help.
What Does Restless Legs Syndrome Feel Like?
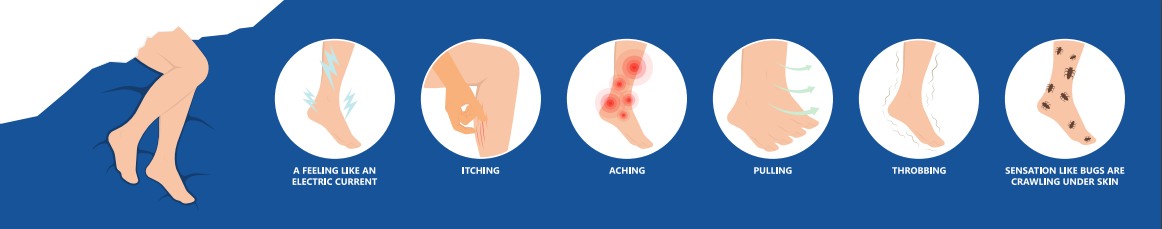
Patients who have Restless Legs Syndrome often have sensations they describe as unpleasant over which they have no control. I've heard the sensation described in the following ways:
- It’s like there were bugs crawling up and down my legs.
- Can feel creepy crawlies I know aren’t there.
- It’s like my skin itches from the inside out. (This is a very common symptom in patients who have venous insufficiency in their lower legs.)
- It’s like I was trying to sleep on pins and needles.
- An electrical buzzing in my legs and body
- I just can’t make my legs stop moving - it’s an uncontrollable urge to move your legs. There’s nothing you can do to make it stop, except get up and walk around.
How is Restless Legs Syndrome Diagnosed?
The diagnosis of RLS is present when these four criteria are present:
- An uncontrolled urge to move the legs with abnormal leg sensations
- The urge begins or worsens with inactivity or rest
- The urge to move is partially or totally relieved by walking
- The urge is worse in the evening or night rather than during the day
People With RLS Often Have the Condition for Some Time Before Diagnosis
Because some of the symptoms of restless leg syndrome overlap with those of other conditions like Parkinson’s disease, diabetic neuropathy, and psychiatric issues, a diagnosis can be difficult. For that reason, it’s important to find out if your RLS is related to a vein condition, and a simple free screening with a vein specialist can rule that out. Many providers, including neurologists, aren’t aware of the advances in the field of vein care that now indicate a relationship between Restless Legs Syndrome and vein reflux. To find out if you have a vein condition causing your RLS, you need to see a vein specialist and get a specialized vein reflux ultrasound. People who have restless legs syndrome have an unusual problem, and they are challenged by the symptoms and sleep deprivation. Restless legs syndrome isn’t a problem that is all in your mind. For many people, it’s caused by a vein circulation condition.
RLS and Vein Conditions Have a Lot in Common
The medical field of epidemiology looks at population statistics to see who gets a disease or symptom, and this helps researchers understand its origin. The patterns seen with Restless Legs Syndrome have striking similarities to the patterns seen with vein reflux, which would be expected if these two are related:
- Both RLS and vein reflux affects women about twice as often as men.
- Women are more likely to develop RLS and vein reflux during pregnancy, and both peak in the third trimester and resolve usually within a month after delivery.
- Sometimes symptoms start before the age of 20, but most of the people who have symptoms bad enough to disrupt their lives are 50 and older.
- RLS and vein reflux both run in families.
- RLS and vein reflux symptoms worsen with age.
- Both vein reflux and RLS predominantly affect the lower legs. Cases of restless arm syndrome are rare; only a dozen are reported in the medical literature.
- RLS and vein reflux tend to appear or worsen in the evening and at night.
- Both RLS and vein symptoms can occur during the day, but both always occur in the evening or at night.
- Both RLS and vein symptoms decrease by the morning for most patients.
- Vein symptoms and RLS both have worsening of their symptoms with rest.
One patient told me she had to sleep in a separate room from her husband because he kicked throughout the night. He wasn’t aware he had RLS, as is frequently the situation - the sleep partner is aware of the restless legs. He also didn’t feel rested in the morning when he woke up. He had vein treatment, successfully resolving his RLS. Both now sleep through the night and feel rested.
What is Vein Reflux and How Does it Relate to Restless Legs Syndrome?
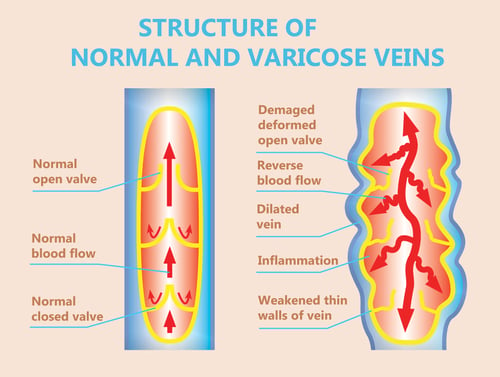
Vein reflux, which is also called venous insufficiency, is a condition in which the blood in the legs is going the wrong way inside the vein. Rather than blood moving from your legs to your heart to get pumped back into circulation, the blood pools in your legs. You can picture this better by thinking of veins as canals for blood. Each vein has several valves that are working to ensure the blood flows the right way. When these valves stop working, it can cause the blood to flow backward, and the valves to fail. Valves that can’t close or that fail will lead to pooled blood in the legs, which will cause pressure and can lead to RLS symptoms. The body reacts to the blood pooling with inflammation in and around the veins. This inflammation causes local symptoms in your legs and feet (such as cramps, RLS, aching, swelling, etc) but also causes generalized fatigue, which happens to be the most common symptom of vein reflux as it advances. While research and knowledge are growing, many providers are not familiar with the relationship between vein reflux and RLS. The only way to get it sorted out is with a vein reflux ultrasound and evaluation by a vein specialist.
In my clinic, 80% of patients with RLS experience an elimination or reduction of their RLS symptoms.
Because vein treatments have such a positive impact on RLS, I recommend vein reflux evaluation in patients with RLS who are not getting relief from medical therapy or who are suffering from side effects of their RLS medications. Each vein treatment will be tailored to your individual condition. If you have vein reflux, the most likely treatment will include closing down abnormally functioning veins where the blood is pooling, and this results in an automatic rerouting of blood flow to healthy, properly working veins. This is due to the fact that your body has an excess number of veins and also continues to make new veins each year. The abnormal veins are then easily reabsorbed into the body. This treatment is called endovenous thermal ablation. Treatments are well tolerated by patients, and most patients note that is way easier than going to the dentist. Patients will need to wear compression stockings for a few days after treatment, but can return to work and resume normal activities including exercise right away.
Other Possible Causes of Restless Legs Syndrome
Medical science does know that these conditions are associated with RLS. The conditions below are not a list of recommended therapies, nor are they confirmed causes. They are conditions that are known to have an association with RLS. I list them because I believe it’s important to be informed. In the cases where a vein condition is not present after a full evaluation, there could be something else at play.
- Kidney disease. Restless leg syndrome is very common in dialysis patients.
- Rheumatoid arthritis. The combination of uncontrollable muscle movement and joint damage can be quite painful.
- Amyloidosis. Amyloidosis is the accumulation of an abnormal protein called amyloid throughout your body.
- Lumbosacral radiculopathy is a fancy way of saying “slipped disc or ruptured disc in your lower back.”
- Iron deficiency. Although low iron is associated with RLS, it also occurs in patients who have hemochromatosis, a condition of iron overload.
- Frequent blood donation. Even if you follow the rules about how often you donate blood, some people become slightly anemic resulting in iron deficiency.
- Magnesium deficiency. Magnesium is a mineral that you get from greens. If you never eat your greens, you may become magnesium deficient.
- Lyme disease. This tick-borne infection can cause numerous neurological issues, including restless leg syndrome.
- Diabetes, both type I and type II. The better you can keep your blood sugar levels under control, the fewer symptoms you will have.
- Vitamin B12 deficiency. Vitamin B12 is an unusual condition, but it can occur in older people who have digestive issues.
- Nicotine, caffeine, or alcohol use. Smoking, drinking alcohol, or drinking coffee, tea, and soft drinks are not causes of restless leg syndrome but may make symptoms worse.
- Neuropathy, especially diabetic neuropathy. Both neuropathy and restless leg syndrome can cause tingling, burning, and creepy-crawly sensations.
- Sjögren syndrome (pronounced show-grin syndrome). Sjögren syndrome is an autoimmune disease that causes white blood cells to build up around glands.
- Sleep problems. Sleep problems make restless leg syndrome worse, and restless leg syndrome makes sleep problems worse.
The long-term health impact of Restless Legs Syndrome can include:
- Sleep Disorder - RLS is a sleep disorder, and people with sleep disorders are known to have a shortened life span.
- Chronic Fatigue - This can be characterized by lowered athletic and work performance, irritability, increased conflict in relationships, and even daytime drowsiness.
- Weight Gain - People with sleep disorders tend to gain weight. Lack of sleep causes fatigue and a feeling of hopelessness or despair, which leads to a lack of exercise or overeating to compensate.
- Quality of Life - Because of the emotional toll of sleeplessness, individuals who suffer from RLS are more likely to experience mood swings, angry outbursts, relationship strain, and more.
- Negative Emotional State - Individuals with RLS can experience depression, hopelessness, despair, irritability, and poor relationships.
There is one additional condition of abnormal leg movements that may be related to RLS and vein reflux: Periodic Limb Movement of Sleep, or PLM. With PLM, there is an involuntary, forceful backward flexing of one foot that lasts from half a second to five seconds every 20 to 40 seconds during sleep. With RLS, the patient is aware of the movement and the sensations and can self-report it to the provider. With PLM, the symptoms occur during sleep so they are not aware of them and they must be reported by the patient’s sleeping partner. The patient just wakes up in the morning feeling washed out and tired. These patients do not report the abnormal sensations seen with RLS.
What Research is Ongoing Relating to Restless Leg Syndrome?
As we have already stated, the direct cause of RLS is still unknown. However, studies are being conducted that point toward a definitive connection between RLS and vein reflux, as well as vein treatment as an effective treatment plan.
- A study published in April 2019 found that there was enough connection and noted improvement in symptoms in RLS patients treated for a vein condition. The study concluded that “Venous ultrasound study and intervention should be considered for potential patients.”

- In another paper published by the National Library of Medicine, the conclusion was that “RLS appears to be a common overlapping clinical syndrome in patients with Chronic Vein Disorder (CVD). In this study, 174 consecutive patients and 174 matched healthy controls. They found that 36% of patients presenting to Phlebology practice had RLS symptoms, and of the 36% that had RLS symptoms - 98% had chronic venous disease. Also, of the 19% of control that had RLS symptoms - 91% had chronic venous disease.
- Kanter Dermatological Surgery 1995 had 113 patients with the dual diagnosis of RLS and varicose veins. They were treated with sclerotherapy only, and of those treated - 98% reported rapid relief.
- Hayes et al Phlebology 2008 studied 35 patients with moderate to severe RLS with CVD. 80% of those with treatment had improvement in their symptoms. 53% had a follow-up score of less than 5 indicating their symptoms had been largely alleviated. 31% had a score of 0 indicating complete relief of their symptoms.
- McDonagh et al COMPASS study Phlebology 2002 studied 186 patients with GSV reflux, 17% with RLS. They were treated with sclerotherapy and 100% reported RLS relief
Other Possible Treatment Options for Restless Legs Syndrome
I would be remiss if I didn’t also offer the additional treatment options available for RLS. That being said, the first thing I would suggest that someone do is schedule a free vein screening to rule out the presence of vein reflux. Where that is the case, treatment for a vein condition is the recommended next step.
Beyond that, here is a list of things people have tried. My patients share a host of things they’ve tried over the years. I keep tabs on those efforts because I’m interested in their efficacy. My professional opinion is that this list doesn’t produce the results that the patients had hoped for, but you are welcome to try them.
- At-Home Treatments: There are many things you can do to eliminate some of the pain associated with RLS without the use of medications they include using heating pads or ice packs, taking hot baths, getting leg massages, or using a specialized vibrating pad such as Relaxis.
- Lifestyle Changes: As previously mentioned, some researchers feel there may be an association between some sort between alcohol, tobacco, and caffeine use and this condition. If you reduce your intake of these substances, it could help reduce your RLS symptoms. In my experience, changes in these habits have not been effective for most patients.
- Folic acid supplementation and iron infusion: There is support among some researchers that these have some benefits, but it isn’t widely accepted.
- Prescriptions, Medications: In some cases, a doctor could prescribe medications like dopaminergic drugs or Mirapex, Neupro, or Requip, which are FDA-approved drugs to treat RLS. They might also prescribe anti-seizure or anticonvulsant drugs like Tegretol, Lyrica, or Neurontin. Be aware, though, that all medications come with many potential side effects, so you will have to discuss the benefits and side effects with your provider. In my experience, there have been a minority of patients who say they have achieved complete resolution of their RLS symptoms through medication.
NOTE: In my experience, there are a handful of patients who say that the medicines work great, but the vast majority that I speak with say it doesn’t work for them...or that they don’t like it because it’s a sedative and causes extreme drowsiness. If you don’t like your medicine because of the side effects, or if you find that taking them isn’t helping, make sure you work with your healthcare provider to back off of them slowly. Many of them need to be tapered off, and can’t be stopped cold turkey without side effects.
If you’ve tried any of these treatments without improvement to your satisfaction, it is likely that your RLS is connected to a vein condition. Schedule a vein reflux ultrasound and an evaluation by a vein specialist to find out.
If you have vein disease, such as venous insufficiency or varicose veins, causing RLS, then understand that simple outpatient vein treatments can help. The results are usually long-lasting, and one can find relief for years before needing another treatment.
Your Next Step
If you are frustrated with RLS and want to see if vein treatments can bring you relief, the only way to do this is to schedule a specialized vein reflux ultrasound and evaluation by a vein specialist. Your next step is easier than you think. We’re happy to answer questions, so feel free to contact us. What you will need is a specialized vein reflux ultrasound, and part of the exam is performed by a qualified vascular ultrasound technician. This is followed by an interpretation of the ultrasound and an assessment of your symptoms by a vein care specialist.
For people that have RLS and we determine also have vein reflux, over 80% will get relief with vein treatments.




